Gastritis is a fairly common disorder, though it is often misunderstood; it is an inflammation of the lining of the stomach. This inflammation, if untreated, may result in complications to health and cause considerable discomfort. Understanding the causes and symptoms of gastritis is important for treating it appropriately.
Types of Gastritis
There are three main types of gastritis:
Acute Gastritis – It suddenly comes on and is mostly because of infections, sometimes excessive alcohol consumption, or the intake of prescribed medicines such as nonsteroidal anti-inflammatory drugs (NSAIDs).
Chronic Gastritis – This type persists over time. It is mostly due to bacterial infection by H. pylori or some autoimmune disorders.
Erosive Gastritis – The most aggressive and debilitating type, it causes erosion on the surface lining of the stomach and may lead to the development of ulcers or haemorrhage.
Common Causes of Gastritis
Several factors can contribute to gastritis, including:
H. pylori infection – A bacterial infection that is one of the leading causes of gastritis.
NSAID overuse – Medications like ibuprofen and aspirin can irritate the stomach lining.
Excessive alcohol consumption – Alcohol weakens the stomach lining, making it more vulnerable to inflammation.
Autoimmune conditions – The immune system mistakenly attacks the stomach lining, leading to chronic inflammation.
What Are the Symptoms of Gastritis? Recognising the Warning Signs
Gastritis symptoms can vary in severity and duration. Some individuals may experience mild discomfort, while others suffer from severe complications requiring immediate medical attention.
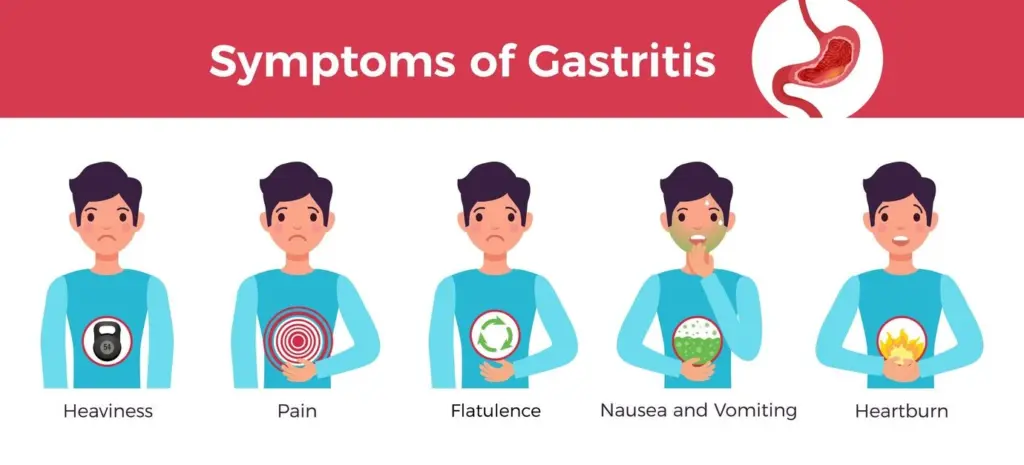
Common Symptoms
Burning or gnawing stomach pain – Usually present in the upper abdomen.
Nausea and vomiting – A recurrent issue, especially after eating.
Bloating and indigestion – Fullness or discomfort after meals.
Loss of appetite – Due to nausea and discomfort, one tends to eat less.
Severe Symptoms (Requiring Urgent Medical Care)
Vomiting blood – Possibly indicating internal bleeding.
Black, tarry stools – Indicates bleeding in the digestive tract.
Dizziness or fainting – Could be caused by major blood loss or dehydration.
Symptoms of Acute Gastritis vs. Chronic Gastritis
Acute gastritis and chronic gastritis, while both affecting the stomach lining, present with different symptoms:
Acute Gastritis – Severe stomach ache, nausea, and vomiting develop suddenly. Acute gastritis may be due to infection, NSAIDs, or alcohol.
Chronic Gastritis – Long-term discomfort with a dull ache, frequent indigestion, and ongoing digestive issues.
How is Gastritis Diagnosed? Tests and Procedures
A diagnosis is essential to treating an ailment; most successful treatments are backed by accurate diagnoses. Different doctors use different methods to diagnose the extent of gastritis, if any.
Diagnostic Procedures
Medical history and physical examination – Doctors assess symptoms, dietary habits, and medication use.
Blood tests – Detect H. pylori infection and check for anaemia.
Stool tests – Identify signs of blood in the digestive system or bacterial infection.
Endoscopy – A small camera is inserted through the throat to examine the stomach lining.
Biopsy – A tissue sample may be taken to rule out more severe conditions like stomach cancer.
What is the Treatment for Gastritis? Medical and Lifestyle Solutions
Effective treatment depends on the cause and severity of gastritis. Medical treatments are often combined with lifestyle changes for better results.
Medical Treatment for Gastritis
Antibiotics – Prescribed for H. pylori infection.
Acid reducers – Include:
Proton pump inhibitors (PPIs) – Such as omeprazole, which reduce stomach acid production.
H2 blockers – Like ranitidine, which decrease acid levels.
Antacids – Provide quick relief from indigestion and stomach pain.
Avoiding NSAIDs – Helps prevent further stomach irritation.
Gastritis Treatment in the UK: NHS Guidelines
The NHS recommends the following treatments for gastritis:
First-line treatment – PPIs and antibiotics if H. pylori infection is present.
Lifestyle modifications – Includes dietary adjustments, reducing alcohol intake, and quitting smoking.
When to see a specialist – If symptoms persist despite treatment or become severe.
Home Remedies and Lifestyle Changes for Gastritis Relief
Making simple lifestyle changes can help manage gastritis and prevent flare-ups.
Dietary Adjustments
Avoid spicy, acidic, or fried foods.
Eat smaller, more frequent meals to reduce stomach strain.
Stay hydrated by drinking plenty of water.
Natural Remedies
Ginger tea – Helps reduce nausea and inflammation.
Probiotics – Support gut health by restoring beneficial bacteria.
Stress management – Practices such as yoga, meditation, and adequate sleep can help prevent flare-ups.
When to Seek Emergency Medical Help
Some symptoms indicate a medical emergency and require immediate attention:
Severe and persistent stomach pain.
Vomiting blood or passing black, tarry stools.
Signs of shock, including pale skin and a rapid heartbeat.
Action: Call 999 or visit A&E immediately if you experience any of these symptoms.
Conclusion: Managing Gastritis Effectively
Gastritis can be managed when diagnosed early and treated appropriately. Improving one’s lifestyle, following the physician’s recommendations, and seeking prompt consultation can help avoid complications.
Call to Action
If there is any persistent abdominal pain or troubling symptom, it is best to consult a doctor without delay.
For more information, visit the NHS gastritis guide.
Chase Lodge Hospital is your premier location for professional care and support in issues of digestive health. Call us for professional medical advice and treatment.